Cancer therapeutics/biotherapeutics are the major sector in the cancer drug market. The market of cancer therapeutics/biotherapeutics is estimated at $210.7 billion in 2025, expected to reach $440.6 billion by 2034, growing at a CAGR of 8.5%. North America dominates the global market with a 45% share in 2023. Europe is anticipated to experience the fastest growth, with a CAGR of 15.8%.
However, over 90% of cancer deaths are linked to drug-resistant cancers. Cancers frequently come to resist to standard-of-care treatments by mutational escape, tumor plasticity, or drug efflux mechanisms. Resistance to EGFR inhibitors in NSCLC, HER2-targeted agents in breast cancer, and chemotherapy in colorectal cancer remains a dominant cause of relapse and mortality. Industry pipelines are now shifting toward new modal approaches beyond traditional chemotherapy and PD-1/PD-1L target immunotherapy.
Palade BioTech develops oncolytic ADC drug, a new type of ADC cancer drug using membrane-destroying Bio-toxins, to solve today’s critical problem in cancer treatment of drug-resistant cancers. Drug resistance in cancer is a major obstacle to successful treatment. Cancer cells can quickly evolve mechanisms to evade the effects of chemotherapy, targeted therapy, and immunotherapy. This leads to treatment failure, cancer progression, and, ultimately, decreased survival rates.
Palade BioTech develops oncolytic AMF drug, a new type of cancer drug using membrane-destroying Bio-toxins, to solve today’s critical problem in cancer treatment of drug-resistant cancers.
Drug-resistant cancers (multi-drug-resistant cancers) are one of the most series and urgent problems. Drug-resistant cancers are currently the culprit for more than 90% of cancer patients. But there are no drugs available at present that can treat drug-resistant cancers effectively.
Therefore, every big pharma is desperate for the development of a new class of drug and toxin to treat drug-resistant cancers. They are looking for new toxins with a new mode of action as no current toxins used in any of the current cancer drug can treat drug-resistant cancers effectively.
The main mechanisms for drug-resistant cancers to occur are 1) over-expression mutations of P-gp / MRP1 pump proteins and 2) loss-of-function mutations of TP53.
Over-expression of P-gp / MRP1 pump proteins can resist to all the currently hot ADC drugs and the traditional chemotherapty drug that are using small molecule toxins payload as the pump proteins pump-out and fail the function of the small molecule toxins.
p53 encoded by TP53 is a master tumor suppressor that leads to cancer cell’s self-killing by apoptosis. All the current cancer drugs including ADC drugs and antibody cancer drugs are ultimately dependent on p53 and apoptosis to kill cancer. Loss-of -function mutants of p53 can evade theses drugs’ cancer killing and drug-resistant cancers occur.
It is extremely difficult to find a toxin that will not be affected by P-gp / MRP1 pump mutants and p53 mutants.
Membrane-disrupting peptide toxins (MD peptide toxins) are ones of the rare toxins that is not affected by P-gp / MRP1 pump mutants and p53 mutants. As membrane-disrupting peptide toxin can cells (normal and cancer cells) physically by destroying the membranes of a cell including the cell surface plasma membrane that envelops a cell, these toxins can kill cancer cells even with P-gp / MRP1 pump mutants and p53 mutants. It is extremely difficult for cancer cells to become resistant to MD peptide toxins.
However, MD peptide toxins destroy not only cancer cells but also normal human cells. MD peptide toxins have intrinsically the human toxicity problem if their membrane-destroying activity is not controlled. This is the reason that no company has succeeded in developing drugs using MD peptide toxins until now even though there were numerous attempts including ones by several big pharmas.
There are several companies on the planet to develop technology to control the membrane-destroying activity of MD peptide toxins. Companies try to reduce their toxicity by diverse masking methods. There are claims that they can control the toxicity of MD peptide toxins. Their technology can reduce 10^3~10^5 folds of the membrane-destroying activity.
MD peptide toxins are extremely toxic in a human body. To resolve the human toxicity problem of MD peptide toxins, we need to be able to reduce more than 10^9 folds of their membrane-destroying activity. This is equivalent to the level such that when you put the gene of a MD peptide toxin into a cell, you can produce the MD peptide without destroying the host cell. No company until now has succeeded in controlling MD peptide’s activity up to this level.
Palade Bio has succeeded for the first time in controlling MD peptide’s activity to the level (more than 10^9 folds reduction) at which MD peptide can be produced in host cells (PaTH/MD Bio-toxin technology). This is a central technology to harness MD peptide toxins for drug development for drug-resistant cancers. The PaTH/MD Bio-toxin technology that harnesses MD peptide toxins is like Enrico Fermi’s Chicago pile 1 that demonstrated the harness of the nuclear power and that was central for the first atomic bomb.
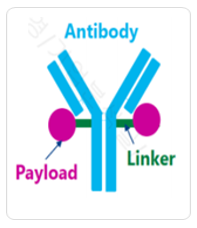

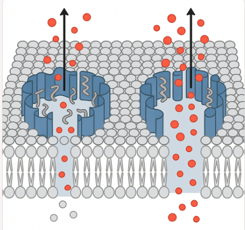
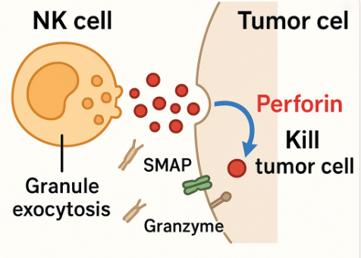
Cancer immunotherapy” is a revolutionary cancer treatment that has recently been established as a major treatment regimen for cancer patients, making a paradigm shift in cancer treatment. Recent trials with cancer immunotherapy have shown successful therapeutic results.
The best observational case of cancer immunotherapy is the treatment of former US President Jimmy Carter’s brain tumor,
which had been considered incurable at the time (2015. Keytruda(pembrolizumab) was an experimental immunotherapy drug at the time.
Thanks to successful treatment with Keytruda, former president Jimmy Carter, the longest-lived US president, passed away in 2024 at 100 years old.
Keytruda(pembrolizumab) is an immuno-therapeutic drug that keeps immune T cells active to kill tumor cells. It was the best-selling blockbuster drug in 2023 and 2024. The annual sales reached 30 billion USD in 2024.
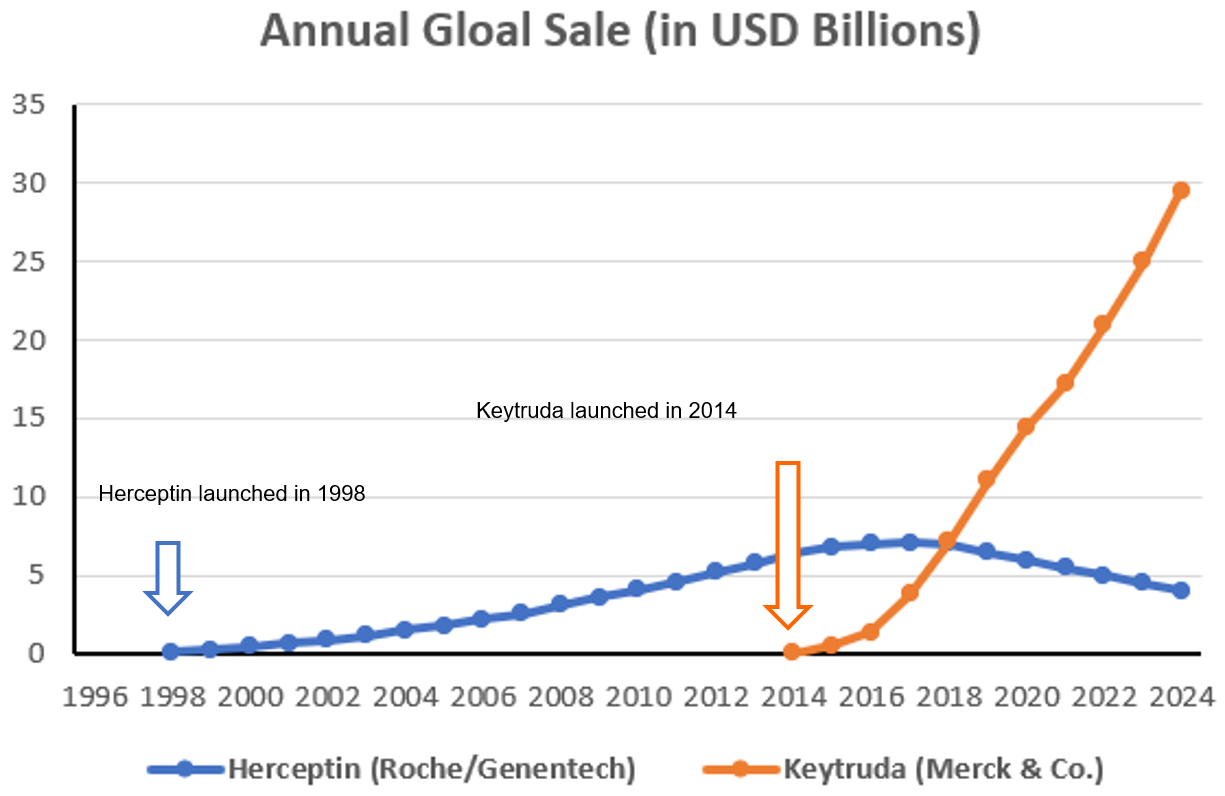
However, Keytruda has a big problem. The majority, 70~85% of cancer patients are non-responsive to Keytruda.
Palade’s oncolytic AMF drug technology will broaden Keytruda’s effectiveness to aa larger number of patients in several ways, including:
Change cold tumors to hot to improve Keytruda effectiveness: Hot tumors are characterized by high mutation loads and significant immune cell infiltration, making them more responsive to immunotherapies like Keytruda. Examples include melanoma, lung cancer, and bladder cancer. Cold tumors tend to have low mutation rates and minimal immune cell presence, making them less responsive to immunotherapy. Common “cold tumor” cancers include ovarian, prostate, and pancreatic cancer. Keytruda is generally more effective in treating hot tumors due to their higher mutation load and immune cell presence, which enhances the drug’s ability to target and destroy cancer cells. Palade’s technology will assist in converting “cold” tumors into “hot” tumors, making treatments like Keytruda more effective.
How Palade’s technology improves treatment efficacy: Most (70~85%) of tumor patients are not responsive to Keytruda if their tumor microenvironment (TME) or tumor immunity microenvironment (TIME) exists normally in a “cold” TME/TIME. Keytruda is most effective if the TME/TIME is “hot.” Research in this field is ongoing, and the exact reasons have not yet been discovered.
Why this matters?
When tumor cells are lysed, they release molecules such as DAMPs, which are immune-activating molecules that convert cold TIME to hot TIME. Puncturing tumor cells can make the patient more responsive to Keytruda, which increases the chance of cure.
Palade develops an adjunct drug in combination with Keytruda using oncolytic AMF drug to increase Keytruda’s responsiveness. Palade develops PaTH 4 hot TIME (Palade Technology Hatching hot Tumor Immunity Micro Environment) technology by application of oncolytic AMF drug that punctures tumor cells to increase the probability of Keytruda’s responsiveness from 15%-30% to over 70%, or higher in some cases. This will be a major advance in the treatment of multiple forms of cancer, like pancreatic.
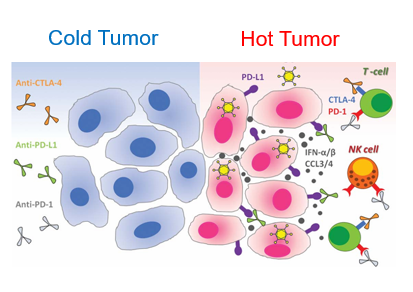
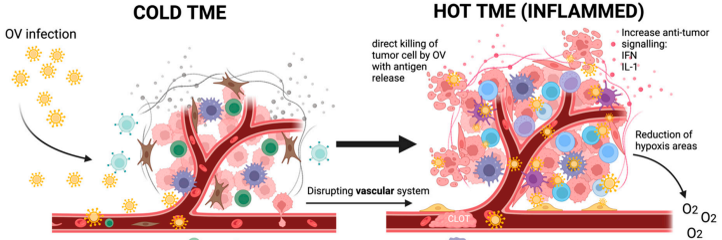
modified from https://www.mdpi.com/1422-0067/25/2/1180
Palade’s cancer immunotherapy goal is to deploy our PaTH 4 hot TIME technology that targets and breaks tumor cells by membrane lysis to convert “cold” tumor immune microenvironment (TIME) into “hot” TIME, which is more sensitive to Keytruda.
Oncolysis (tumor cell lysis) releases immune-activating molecules, DAMPs, which convert cold TIME to hot TIME. These cells can convert tumor growth-favoring, pro-tumor TIME (tumor immunity microenvironment) (cold TIME) into tumor growth-preventing, anti-tumor TME (hot TIME).
Our “tumor immune microenvironment (TIME) modulator drugs” using the PaTH 4 hot TIME technology will be used as a combination drug with Keytruda for tumor immunotherapy to enhance the patient’s sensitivity to Keytruda.
Cold TME is predominantly composed of Treg, MDSC, CAF and TAM2 cells that protect tumor cells (pro-tumoric microenvironment) while hot TME is composed of CD4 or CD8 T cells, NK, DC, M1 cells that attach and kill tumor cells (anti-tumoric microenvironment).
Using our oncolytic ADC drug technology, Palade BioTech develop “molecular precision scalpel by targeted killing and removing the invisible, remaining cancer cells after cancer surgery.
Palade BioTech will develop additional GPCR-target drugs to the GPCR-target tumor microenvironment modulator drugs using our MoSTT-CelSuR platform technology. We will focus on GPCR-target drugs metabolic diseases and anti-aging.
With a bold vision to become a global leader in resistance-targeted therapeutics, we are pioneering curative solutions for drug-resistant, immunotherapy-refractory cancers and incurable viral threats, the areas of highest mortality and unmet need.